Why Hybrid?
Persistent AFib Is Different.
If atrial fibrillation (AFib) persists for more than 12 months despite treatment, it is classified as longstanding persistent AFib (LSPAF).
Patients with LSPAF face a significantly different reality compared to those with early or paroxysmal AFib. Up to 50% of patients may have LSPAF, and many are unaware that they have the condition OR how long, until they experience a stroke, heart failure, or another clotting-related issue.
To address this, the Hybrid AF Converge Trial was initiated to explore the combination of catheter ablation and surgical ablation techniques. The results of the trial were subsequently approved by the FDA, leading to the development of what is now known as Hybrid AF therapy.
Catheter ablation success rates decline significantly with time
Recurrence rates increase over time
Structural remodeling and scarring of the left atrium progress
Medication dependency often continues
Stroke risk and heart failure risk can rise
Studies now show that persistent AFib can be treated safely and with improved outcomes using a comprehensive epicardial + endocardial strategy—not just another pass with the catheter inside the heart.
Evidence-Based Reality
- Single catheter ablation success rates can be as low as 20–45% at 1–2 years in longstanding persistent AFib
- Multiple repeat procedures are often required
- Antiarrhythmic medications frequently continue long-term
- Anticoagulation often remains lifelong despite ablation
If you have been told, “We’ve done all we can,” or “There’s nothing else,” hybrid convergent therapy may offer a different path.
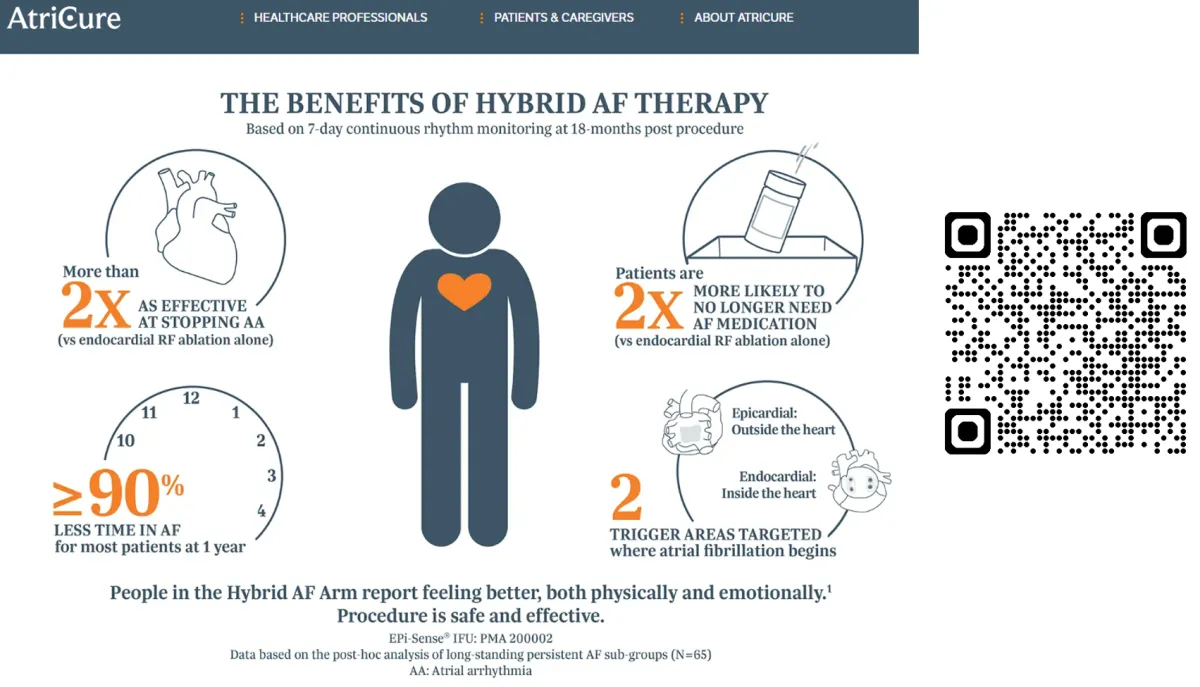
A Real Disease Requires A Real Treatment Strategy
The Hybrid Convergent Procedure
Two Teams. One Strategy. Superior Rhythm Control.
Hybrid convergent therapy combines minimally invasive surgical ablation on the outside of the heart with advanced electrophysiology mapping on the inside. The goal: durable sinus rhythm in patients with longstanding AFib (LSPAF).
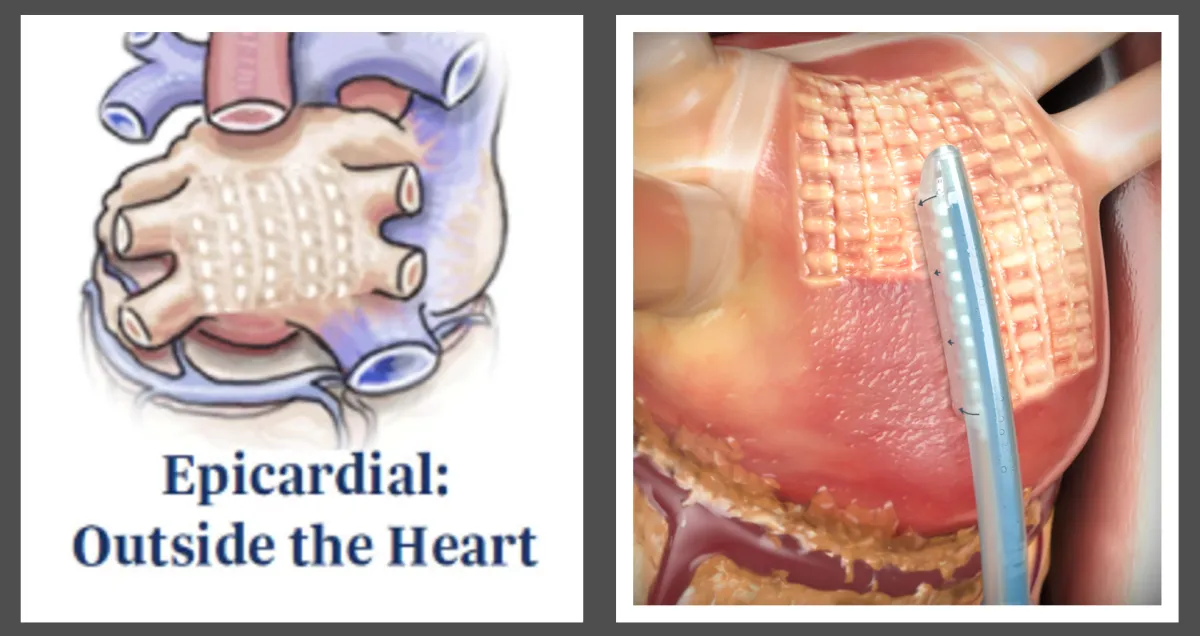
Step 1 – Surgical Epicardial Ablation
Minimally invasive VATS or robotic approach
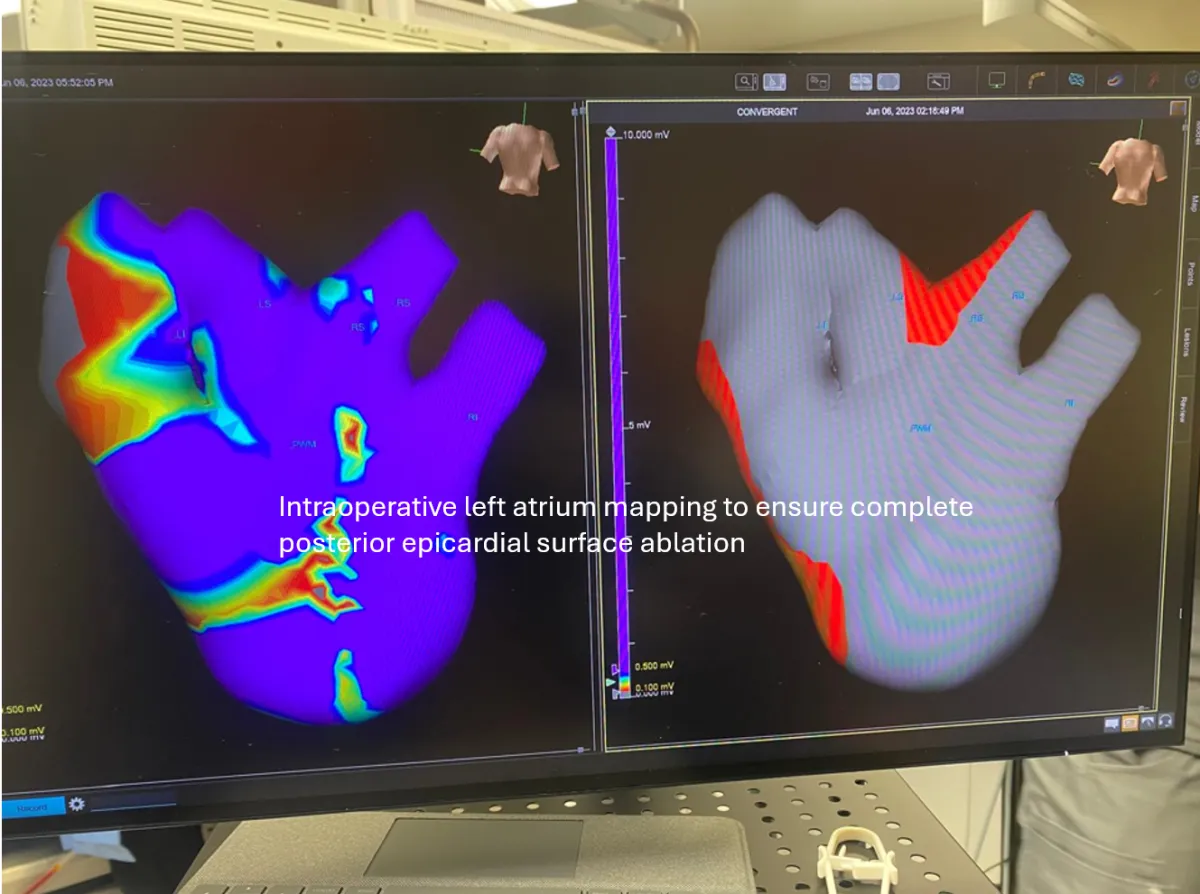
Posterior left atrial ablation using EPiSense™ system
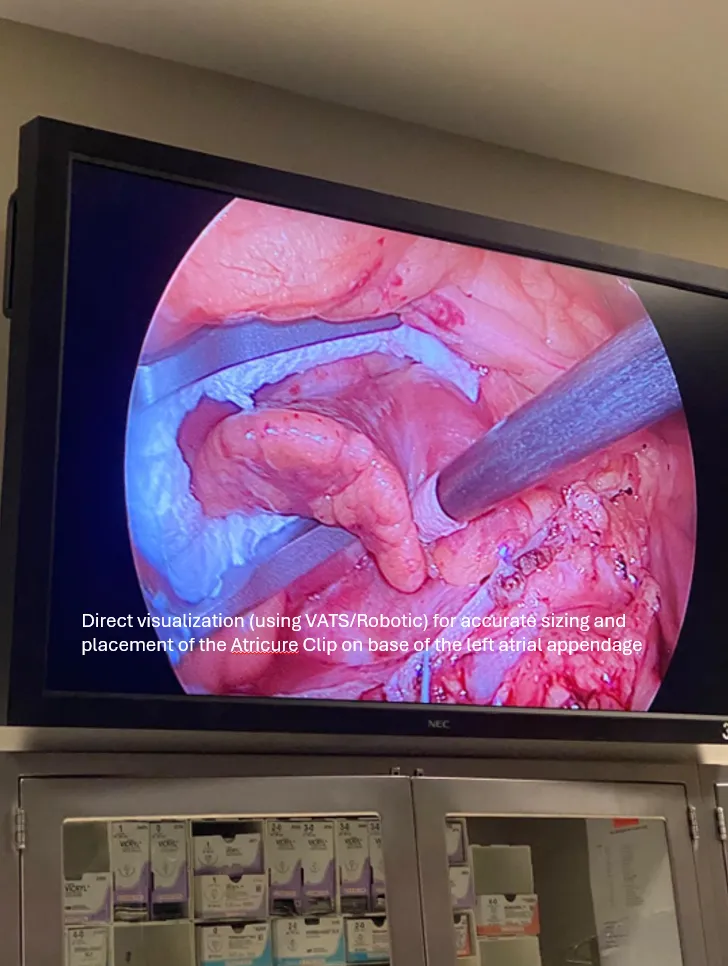
Left atrial appendage ligation
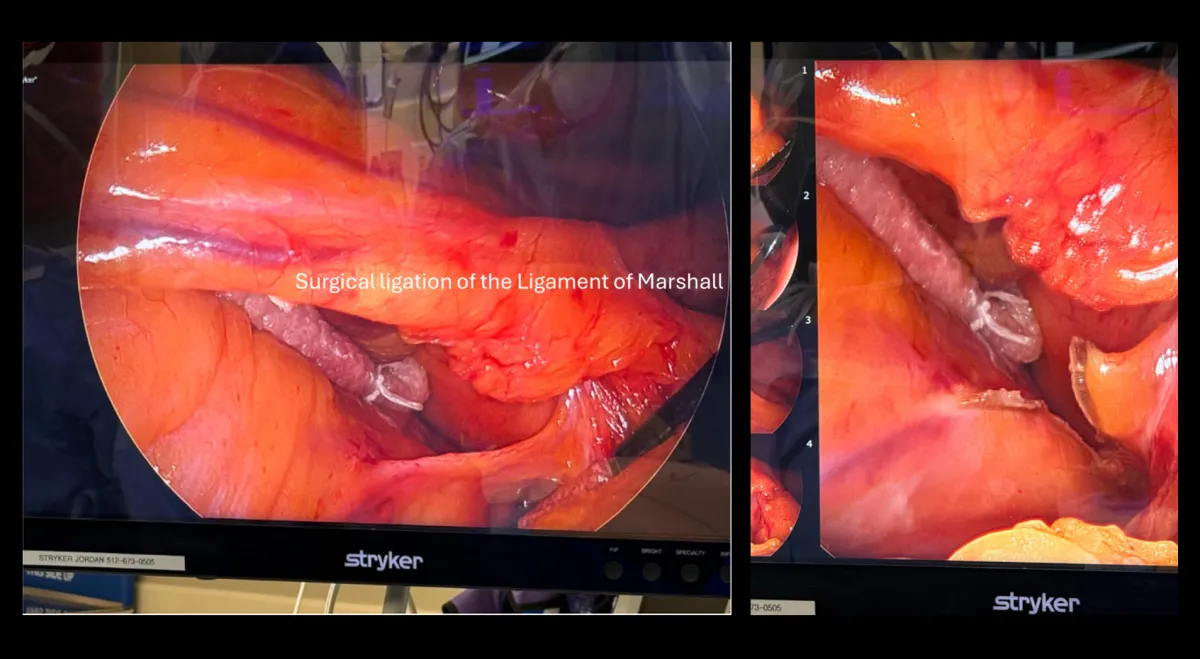
Ligament of Marshall division
Roof line creation and posterior wall debulking
Electrical cardioversion under general anesthesia if needed
By addressing the epicardial substrate on the back wall of the left atrium, this step targets areas often missed by endocardial catheter ablation alone.
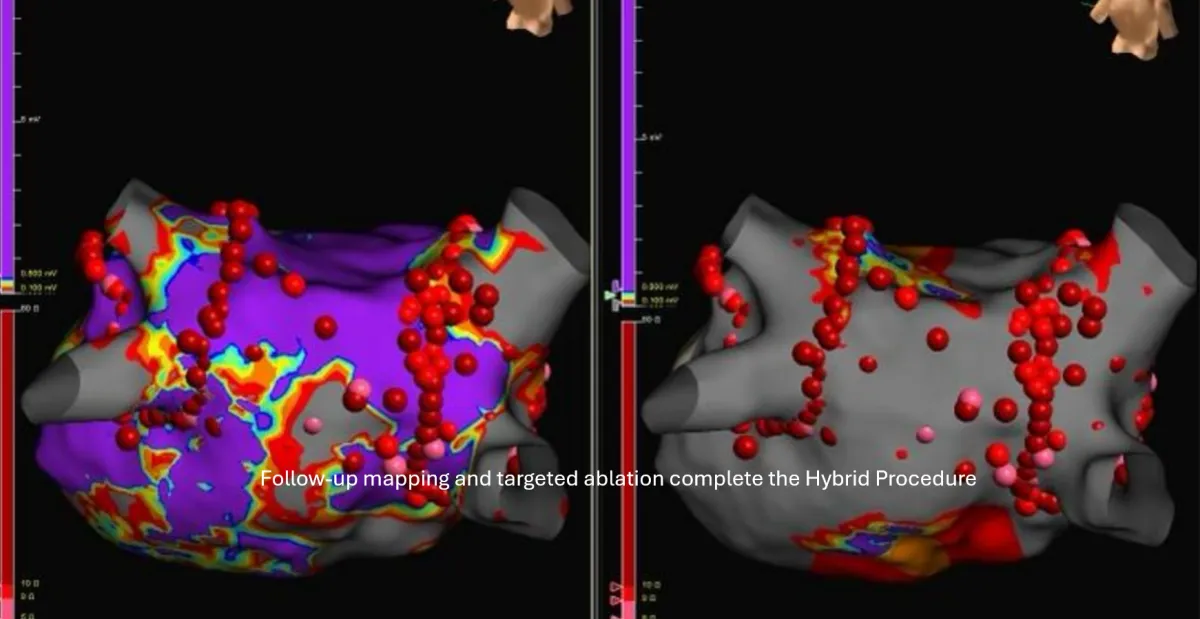
Step 2 – Electrophysiology Mapping (4–6 Weeks Later)
- Endocardial catheter mapping of left atrium
- Completion of lesion sets and touch-up ablation
- Electrical isolation confirmation of pulmonary veins and posterior wall
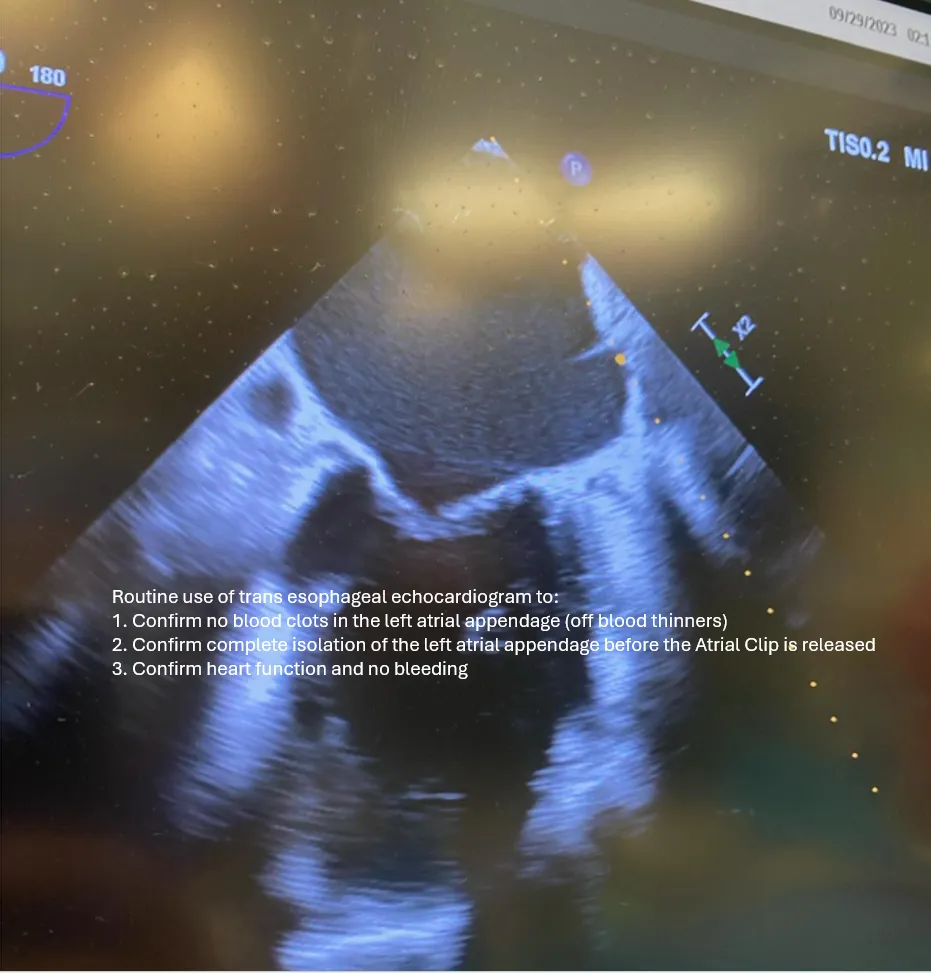
- Verification of left atrial appendage exclusion and conduction block
This staged, collaborative approach allows the EP team to fine-tune rhythm control and confirm durability of the surgical lesions.
Why It Works Better
Targets posterior wall substrate not reliably reached with catheter alone
Addresses non-pulmonary vein triggers and complex circuits
Improves rhythm durability in enlarged or remodeled atria
Safely treats left atrial appendage as a potential source of AFib and stroke
Clinical trials and multicenter registries show:
- Up to ~65–80% freedom from AFib at 2 years
- Significant reduction in antiarrhythmic medications
- Many patients able to discontinue anticoagulation after evaluation
- Higher rhythm durability versus catheter ablation alone in persistent AFib

What Patients Can Expect
Our Lake Charles hybrid AFib program is designed around predictable recovery, clear communication, and long-term rhythm success.
Hospital Stay
1–3 Days
Most patients go home within 1–3 days after the surgical portion of the hybrid procedure.
Pain
Minimally Invasive
Most patients report mild to no discomfort that improves quickly with our enhanced recovery protocols.
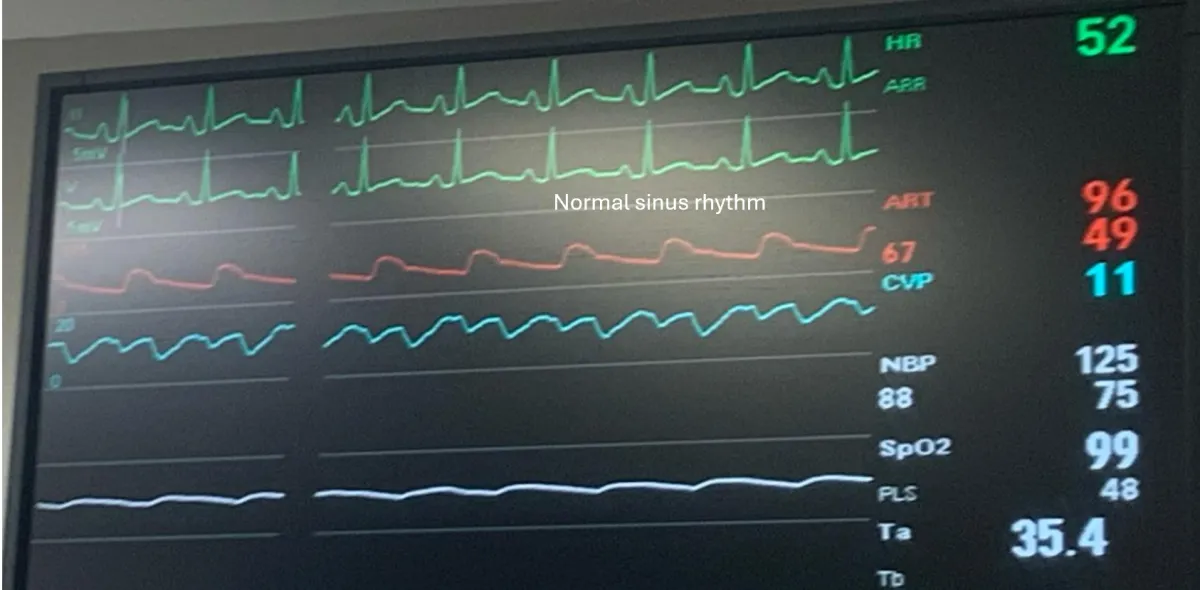
Rhythm at Discharge
80–90% in Sinus
In many hybrid programs, up to 90% of patients leave the hospital in sinus rhythm after the convergent procedure.
Long-Term Goals
- Durable sinus rhythm
- Reduced medication burden
- Lower stroke risk when appropriate
- Improved exercise tolerance and quality of life
Who Is a Candidate?
Hybrid convergent therapy is built for complex, longstanding AFib—including many patients who have been turned down for repeat procedures elsewhere.
We do not turn away complex patients without a complete, individualized evaluation.
- AFib lasting > 12 months (longstanding persistent AFib)
- Failed prior catheter ablation or cardioversions
- Medication-refractory AFib with symptoms or intolerance
- Enlarged left atrium or structural remodeling
- Obesity with AFib; diabetes and metabolic syndrome
- High-risk patients previously declined for repeat ablation
- Patients seeking alternatives to lifelong rhythm drugs and blood thinners
We review prior records, imaging, and rhythm data and coordinate with your local cardiologist or EP when appropriate.
The ABCDE+S Optimization Framework
Because Rhythm Control Alone Is Not Enough.
We optimize the whole patient before and after surgery—focusing on metabolic health, vascular stability, inflammation, and early detection. This is not just a procedure; it is a rhythm + longevity program.
A – A1C
GLP-1 pathway support and metabolic reset to improve insulin sensitivity and reduce AFib-driving inflammation.
B – Blood Pressure
Tight vascular and hemodynamic control to reduce wall stress, stroke risk, and AFib triggers.
C – Cholesterol
Plaque stabilization and lipid strategy to protect coronary circulation and cerebral perfusion.
D – Diet
Anti-inflammatory nutrition and weight management tailored to cardiac and metabolic risk.
E – Exercise
Graduated cardiac conditioning programs aligned with rhythm status and structural findings.
S – Screening
Coronary calcium scoring, lung cancer CT when indicated, age-based cancer screening, and sleep apnea evaluation.
Calculate YOUR CHA₂DS₂-VASc Score for Atrial Fibrillation Stroke Risk
Calculates stroke risk for patients with atrial fibrillation (QR code) and new STAGES of Atrial Fibrillation by ACC.
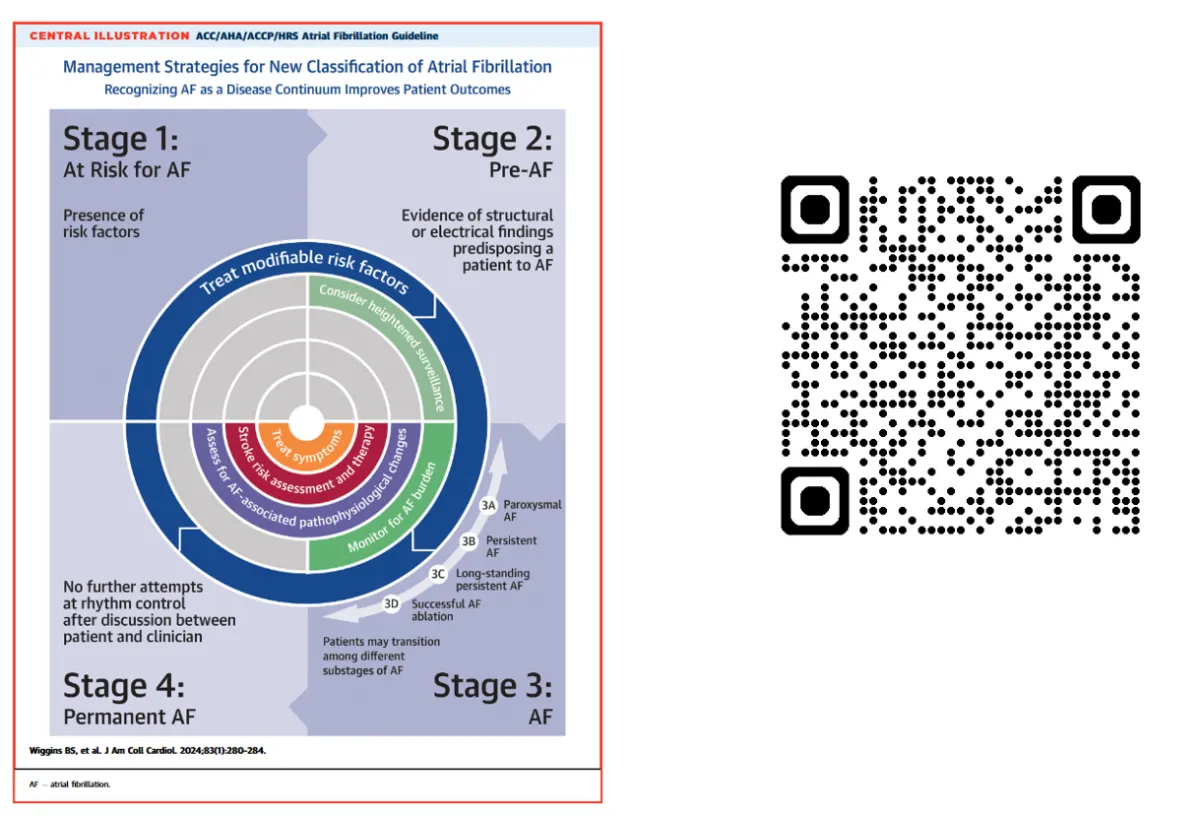
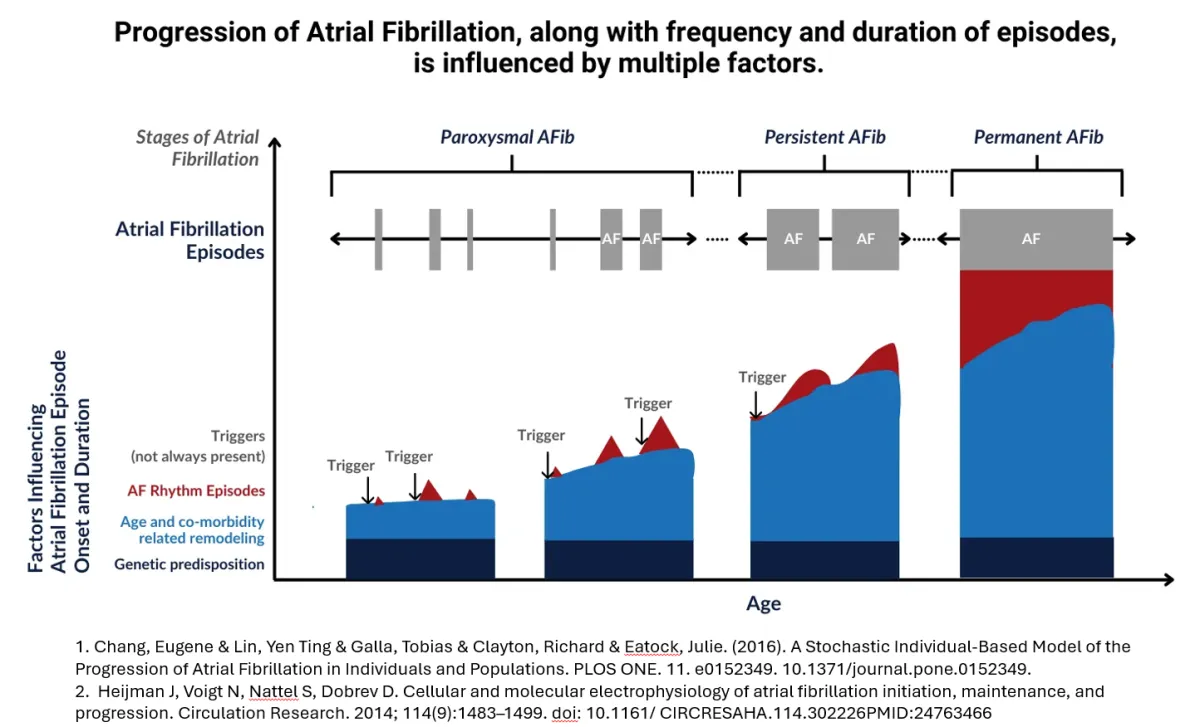
Destination AFib Care – Lake Charles, Louisiana
Access advanced hybrid AFib convergent therapy without the congestion, cost, and chaos of a big-city medical center. Lake Charles offers a unique blend of resort-level comfort and evidence-based care.
Within ~600-mile Radius
- Houston, Dallas, San Antonio
- Baton Rouge, New Orleans
- Mississippi Gulf Coast
- Alabama Gulf Coast
- Florida Panhandle
International patients welcome with dedicated coordination and telehealth pre-screening.
What We Provide
Concierge coordination and a dedicated AFib travel coordinator
Pre-operative telehealth evaluations and record review
Lodging and resort guidance near Lake Charles casinos and waterfront
Post-op remote rhythm monitoring and telehealth follow-up if needed
Coordination with your local cardiologist / electrophysiologist
Our team will outline travel timing, length of stay, and follow-up options tailored to your situation.

Director, Cardiothoracic Surgery Services, CHRISTUS Ochsner Health, Lake Charles, Louisiana
About Dr. Daniel L. Beckles, MD, PhD
Double-Boarded Cardiothoracic Surgeon & Minimally Invasive Thoracic Specialist
Dr. Beckles brings more than 30 years of surgical experience to Gulf Coast Hybrid AFib Center, with a career focused on precision surgery, minimally invasive thoracic approaches, and prevention-driven care.
- American Board Certified in General Surgery and Thoracic Surgery
- Fellowship-trained in minimally invasive thoracic surgery
- Leader in hybrid AFib and convergent techniques
- Expertise in VATS and robotic approaches
- Reduced pain, shorter length of stay philosophy
- Integrated metabolic and longevity medicine mindset
Philosophy: Precision surgery. Metabolic optimization. Longevity medicine. Every convergent procedure is part of a larger plan to extend healthspan, not just suppress an arrhythmia.
Frequently Asked Questions
Straightforward answers to the most common questions about hybrid convergent therapy, blood thinners, and recovery expectations.
Is the convergent hybrid procedure FDA approved?
Yes. The convergent procedure platform used in our hybrid AFib program is FDA approved. We follow guideline-based protocols and review all risks and benefits with you before scheduling. FDA approval was in 2021.
Will I be able to stop blood thinners (anticoagulation)?
Many patients may qualify to discontinue blood thinners after rhythm stabilization and secure management of the left atrial appendage. This decision is individualized based on your stroke risk score (CHA₂DS₂-VASc), imaging, and shared decision-making with your cardiologist. Up to 80% of patients are off anticoagulation meds after their Hybrid AF Ablation.
What if I failed catheter ablation before?
You may actually be an ideal candidate. Hybrid convergent therapy was designed precisely for patients with persistent or longstanding AFib who have not responded to catheter ablation alone. The surgical approach addresses areas of the heart catheter cannot access.
Is this open-heart surgery?
No. The convergent procedure is performed through small incisions using minimally invasive thoracoscopic or robotic approaches. The heart is not stopped and there is no sternotomy.
How long is recovery?
Most patients are walking the hallway the day after surgery and resume light activity within days. Return to work and heavier activity depends on your baseline health and job type, and is decided collaboratively with your care team. Some patients are discharged the next day after surgery.

For Cardiologists & Electrophysiologists
A Collaborative Hybrid AFib Destination Center on the Gulf Coast
We operate as an extension of your practice, not a competitor. Our hybrid program is designed for longstanding persistent AFib, redo ablations, and high-risk patients seeking a durable rhythm strategy.
- Collaborative model with shared care pathways
- Patients returned to the referring cardiologist post-procedure
- Detailed operative, EP mapping, and follow-up reports
- Access to CONVERGE-style protocols and multicenter best practices
- Options for joint teleconferences and case review
Hybrid Data Packet
We provide a concise evidence packet you can review or share with your group.
- CONVERGE trial summary
- Multicenter registry outcomes
- Comparison: catheter vs. hybrid convergent
- Suggested selection criteria & workflow
Request the digital packet or schedule a case review conference.
Data & Clinical Evidence
Hybrid Convergent vs. Catheter Ablation Alone
Our experience and program is built on the CONVERGE trial, multicenter registries, and real-world data showing meaningful improvements in rhythm control for longstanding persistent AFib.
Key Evidence Highlights
- CONVERGE Trial: Hybrid convergent therapy demonstrated superior freedom from atrial arrhythmias vs. endocardial catheter ablation alone in persistent/longstanding persistent AFib.
- Multicenter registries: Report ~65–80% freedom from AFib at ~2 years in carefully selected patients.
- Stroke reduction: Left atrial appendage management plus rhythm control may reduce stroke risk when combined with appropriate anticoagulation strategies.
- AFib recurrence: Lower need for multiple repeat ablations compared with endocardial catheter-only strategies in this population.
Hybrid AFib Consultation Center
Take the Next Step Toward Freedom from AFib
Share your history, prior procedures, and current medications. Our AFib team will review your case and coordinate the next best step—locally, nationally, or internationally.
Location: 401 Dr. Michael Debakey Drive, Lake Charles, Louisiana
Phone: (337) 513-0105
- Telehealth consultations available for qualifying patients
- Secure upload portal for prior records and rhythm strips
- Coordinated scheduling for out-of-town and international patients
Persistent AFib Is Not a Life Sentence.
There is another option. Hybrid Convergent Therapy • Lake Charles, Louisiana
Gulf Coast Hybrid AFib Center • Minimally Invasive Convergent AFib Procedure • Lake Charles, Louisiana • Serving Louisiana, Texas, and international patients.